Does Holiday Heart Syndrome, which affects the atria, extend to the ventricles?
In an extensive study of more than 400,000 individuals, investigators found no association between alcohol consumption and ventricular arrhythmias, although higher spirit intake was associated with increasing risk, finds a new report in Heart Rhythm.

Philadelphia, December 21, 2021 — The relationship between alcohol and atrial fibrillation has long been referred to as the Holiday Heart Syndrome. An extensive study of the relationship between total alcohol consumption and cardiovascular disease determined that this phenomenon is not associated with ventricular arrhythmias (VAs). It appears in Heart Rhythm, the official journal of the Heart Rhythm Society, the Cardiac Electrophysiology Society, and the Pediatric & Congenital Electrophysiology Society, published by Elsevier.
Researchers analyzed data from the UK Biobank, a large-scale research database with health information collected from half a million UK volunteers, to assess baseline alcohol consumption reported by more than 408,000 participants as a predictor of VAs and sudden cardiac deaths (SCDs) over a median follow-up of 11.5 years. They characterized associations of total and beverage-specific alcohol consumption with incident VA and SCD.
“This is one of the first studies to specifically investigate the relationship between long-term alcohol consumption and VA,” explained lead investigator Christopher X. Wong, MBBS, MSc, PhD, Centre for Heart Rhythm Disorders, University of Adelaide and Royal Adelaide Hospital, Adelaide, Australia. “We sought to clarify the relationship between alcohol consumption and two types of cardiovascular disease: VAs, which are often life-threatening abnormal heart rhythms; and SCDs, which are deaths that were thought to be caused by a loss of heart function and can often be due to VA.”
In this predominantly white British cohort, no association was observed between total alcohol, beer, cider, or red or white wine consumption and VA risk. Of note, individuals who consumed at least 14 drinks per week of spirits, but not other types of alcohol, did experience a roughly 20% higher risk of VAs.
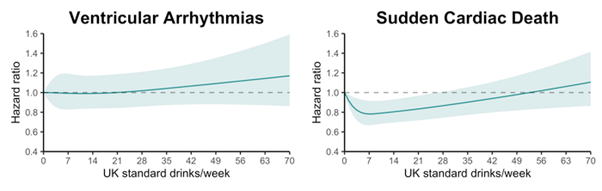
Investigators determined that the relationships between alcohol consumption and VA and SCD were quite different. They observed a U-shaped association between alcohol consumption and risk of SCD, consistent with prior studies. This was unexpected because it is often assumed that SCDs are due to VA. Although VAs can cause SCDs, not all SCDs are caused by VAs. In fact, some SCDs are actually thought to be due to conditions unrelated to the heart, and this may explain what appears to be a different effect of alcohol on these similar conditions.
“Previous studies have looked at the association of alcohol and SCD and have observed a protective association at lower levels of alcohol intake. Yet, we know that diagnoses of SCD and VA are not equivalent, and that a sizeable minority of what we believe to be sudden cardiac deaths are actually deaths due to non-cardiac causes,” added Dr. Wong.
Dr. Wong emphasized that the investigators do not recommend that people drink for their heart health. “In our opinion, there is insufficient evidence to recommend that non-drinkers consume alcohol for health benefits. We also know that alcohol consumption increases the risk of bowel and breast cancer and causes damage to the liver. Therefore, the effect of alcohol on health should be viewed in its entirety when we make safe alcohol consumption recommendations.”
The investigators also stress that these findings require clarification in further epidemiological and experimental studies with accurately defined VA and SCD events.
In an accompanying editorial, Stacey J. Howell, MD, and Gregory M. Marcus, MD, MAS, FHRS, from the Section of Electrophysiology, Division of Cardiology, University of California, San Francisco, San Francisco, CA, USA, comment that, “The current study does not appear to provide compelling evidence that the Holiday Heart Syndrome extends to the ventricles, indeed demonstrating that moderate alcohol consumption may protect against SCD. It is worth noting that, in excess, alcohol consumption generally increased the risk of SCD. Despite a common belief that alcohol is generally heart-healthy, this fits with previous evidence that excess alcohol even increases the risk for myocardial infarction, demonstrating that ‘more is not better.’”
According to the Centers for Disease Control and Prevention (CDC), excessive alcohol use led to approximately 95,000 deaths and 2.8 million years of potential life lost each year in the United States from 2011 to 2015, shortening the lives of those who died by an average of 29 years. The economic costs of excessive alcohol consumption in 2010 were estimated at $249 billion. Over time, excessive alcohol use can lead to the development of chronic diseases such as high blood pressure, heart disease, stroke, liver disease, and digestive problems, as well as several types of cancer.
Understanding the role of alcohol in cardiovascular diseases and other health issues can help inform guidelines for safe alcohol consumption. Each country has its own alcohol consumption recommendations, and the size of a standard drink also differs between countries. In the United States, for example, one standard drink contains 14 grams of alcohol; the CDC recommends consumption of no more than seven US-sized standard drinks (98g alcohol) per week in women and no more than 14 US-sized standard drinks (196g alcohol) per week in men. In the United Kingdom, one standard drink contains eight grams of alcohol, and the National Health Service (NHS) recommends no more than 14 UK-sized standard drinks (98g alcohol) per week in both women and men.
IMAGE: INVESTIGATORS DETERMINED THAT THE RELATIONSHIPS BETWEEN ALCOHOL CONSUMPTION AND VENTRICULAR ARRHYTHMIAS AND SUDDEN CARDIAC DEATH WERE QUITE DIFFERENT. LEFT: ASSOCIATION OF TOTAL ALCOHOL CONSUMPTION AND INCIDENT VENTRICULAR ARRHYTHMIAS; RIGHT: ASSOCIATION OF TOTAL ALCOHOL CONSUMPTION AND SUDDEN CARDIAC DEATH. view more
CREDIT: HEART RHYTHM